Genetic Information
Gene & Transcript Details
| ID | Status | Details |
|---|---|---|
| NM_003620.3 | RefSeq Select | 4790 nt | 233–2050 |
| NM_003620.4 | MANE Select | 4768 nt | 223–2040 |
| NM_003620.2 | Alternative | 3163 nt | 223–2040 |
Variant Details
Clinical & Population Data
Population Frequency
gnomADClinVar
Open""
COSMIC Somatic Evidence
Open
Functional Impact & Domains
Functional Domain
The PPM1D L538* variant is functionally characterized as a truncating mutation that confers gain-of-function activity. It results in a C-terminally truncated protein associated with increased protein stability and attenuated activation of DNA damage response mediators such as p53 and H2AX. Functional studies demonstrate that cells with this mutation exhibit increased growth and colony formation, reduced phosphorylation of CHK2 and p53, and resistance to chemotherapeutic agents. In vivo mouse models show that these truncating mutations lead to increased development of acute myeloid leukemia following ionizing radiation exposure. These findings support a damaging, oncogenic effect of the PPM1D L538* variant.
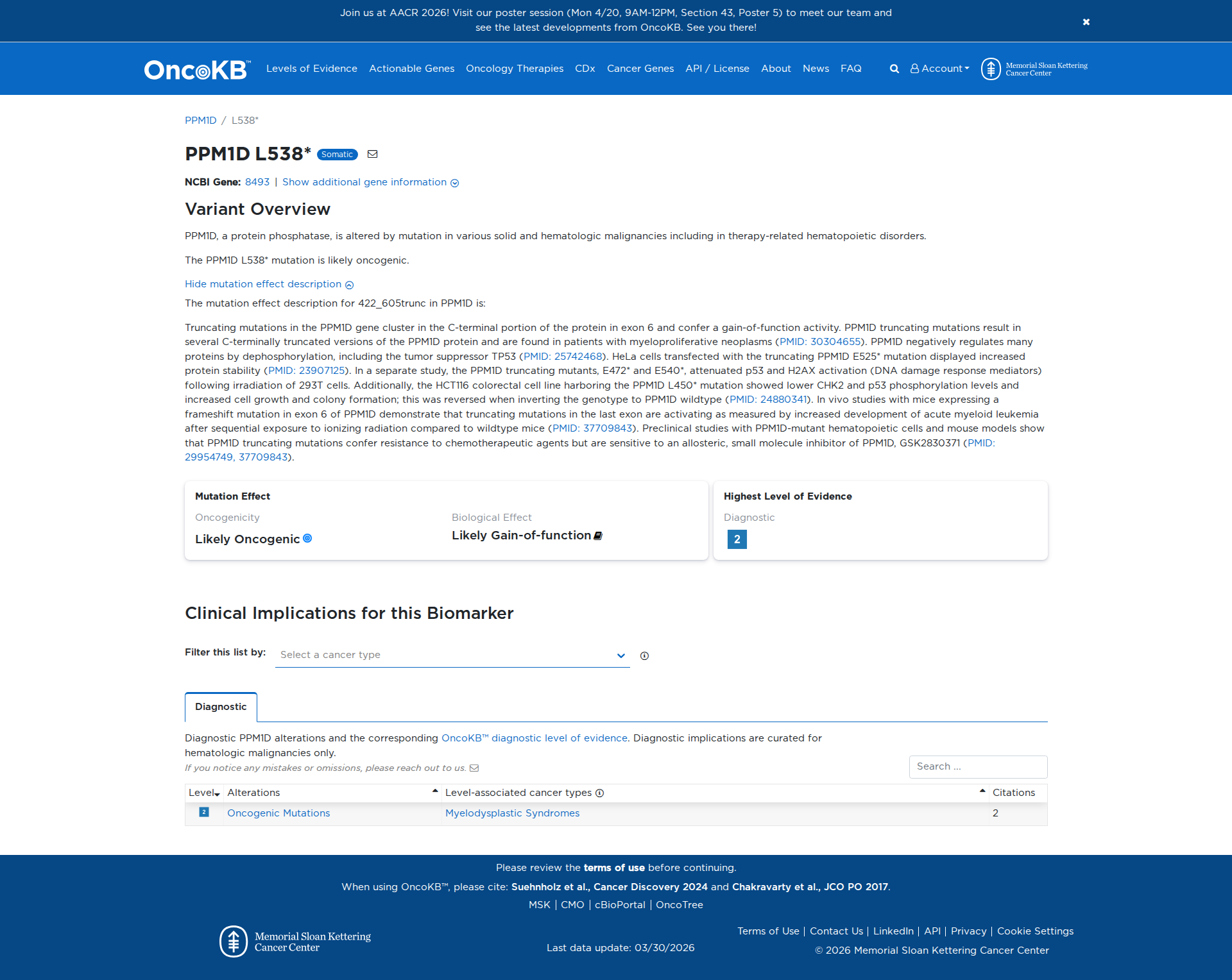
Click on previews to view full database entries. External databases may require institutional access.
Computational Analysis
Pathogenicity Predictions
SpliceAISpliceAI Scores
Window: ±500bp| Effect Type | Score | Position |
|---|---|---|
| Acceptor Loss (AL) | 0.0 | -350 bp |
| Donor Loss (DL) | 0.0 | -485 bp |
| Acceptor Gain (AG) | 0.0 | -341 bp |
| Donor Gain (DG) | 0.0 | -294 bp |
VCEP Guidelines
Applied ACMG/AMP Criteria (VCEP Specific)
PVS1 (Not Applied)
According to standard ACMG guidelines, the rule for PVS1 is: 'Null variant (nonsense, frameshift, canonical ±1 or 2 splice sites, initiation codon, single or multi-exon deletion) in a gene where loss of function is a known mechanism of disease (Very Strong)'. The evidence for this variant shows c.1613del (L538*) generates a truncating protein that confers gain-of-function activity rather than loss of function, and loss of function is not the disease mechanism for PPM1D. Therefore, this criterion is not applied.
PS1 (Not Applied)
According to standard ACMG guidelines, the rule for PS1 is: 'Same amino acid change as a known pathogenic variant but different nucleotide change (Strong)'. There is no known pathogenic variant that results in L538* by a different nucleotide change. Therefore, this criterion is not applied.
PS2 (Not Applied)
According to standard ACMG guidelines, the rule for PS2 is: 'De novo (both maternity and paternity confirmed) in a patient with the disease and no family history (Strong)'. The de novo status of this variant is unknown. Therefore, this criterion is not applied.
PS3 (Strong)
According to standard ACMG guidelines, the rule for PS3 is: 'Well-established in vitro or in vivo functional studies supportive of a damaging effect on the gene or gene product (Strong)'. The evidence for this variant shows that truncating L538* confers gain-of-function activity, increases protein stability, attenuates activation of DNA damage response, promotes cell growth and colony formation, and predisposes to acute myeloid leukemia in mouse models. Therefore, this criterion is applied at Strong strength because multiple functional studies demonstrate a damaging (oncogenic) effect.
PS4 (Not Applied)
According to standard ACMG guidelines, the rule for PS4 is: 'Prevalence in affected individuals significantly increased compared with controls (Strong)'. There are no case-control data demonstrating significantly increased prevalence in affected individuals. Therefore, this criterion is not applied.
PM1 (Not Applied)
According to standard ACMG guidelines, the rule for PM1 is: 'Located in a mutational hotspot or well-established functional domain without benign variation (Moderate)'. While truncating variants in the last exon of PPM1D are recurrent, no VCEP-approved hotspot rule exists and benign variation data are lacking. Therefore, this criterion is not applied.
PM2 (Moderate)
According to standard ACMG guidelines, the rule for PM2 is: 'Absent from controls (or at extremely low frequency if recessive) (Moderate)'. The evidence for this variant shows it is absent from population databases including gnomAD (MAF=0%). Therefore, this criterion is applied at Moderate strength.
PM3 (Not Applied)
According to standard ACMG guidelines, the rule for PM3 is: 'Detected in trans with a pathogenic variant for a recessive disorder (Moderate)'. PPM1D-related disease is dominant and phase information is not applicable. Therefore, this criterion is not applied.
PM4 (Not Applied)
According to standard ACMG guidelines, the rule for PM4 is: 'Protein length changes due to in-frame deletions/insertions or stop-loss variants (Moderate)'. This variant is a frameshift that introduces a premature stop, not an in-frame change. Therefore, this criterion is not applied.
PM5 (Not Applied)
According to standard ACMG guidelines, the rule for PM5 is: 'Novel missense change at an amino acid residue where a different pathogenic missense change has been seen (Moderate)'. This variant is truncating, not missense. Therefore, this criterion is not applied.
PM6 (Not Applied)
According to standard ACMG guidelines, the rule for PM6 is: 'Assumed de novo, but without confirmation of paternity and maternity (Moderate)'. There is no de novo evidence. Therefore, this criterion is not applied.
PP1 (Not Applied)
According to standard ACMG guidelines, the rule for PP1 is: 'Co-segregation with disease in multiple affected family members (Supporting)'. No segregation data are available. Therefore, this criterion is not applied.
PP2 (Not Applied)
According to standard ACMG guidelines, the rule for PP2 is: 'Missense variant in a gene with a low rate of benign missense variation and where missense variants are a common mechanism of disease (Supporting)'. This variant is truncating, not missense. Therefore, this criterion is not applied.
PP3 (Not Applied)
According to standard ACMG guidelines, the rule for PP3 is: 'Multiple lines of computational evidence support a deleterious effect on the gene/gene product (Supporting)'. Computational tools (SpliceAI, etc.) do not predict deleterious effects on splicing or function. Therefore, this criterion is not applied.
PP4 (Not Applied)
According to standard ACMG guidelines, the rule for PP4 is: 'Patient’s phenotype or family history highly specific for a disease with a single genetic etiology (Supporting)'. No phenotype or clinical presentation data are provided. Therefore, this criterion is not applied.
PP5 (Not Applied)
According to standard ACMG guidelines, the rule for PP5 is: 'Reputable source reports variant as pathogenic, but without accessible evidence (Supporting)'. The variant is not reported in ClinVar or other databases. Therefore, this criterion is not applied.
BA1 (Not Applied)
According to standard ACMG guidelines, the rule for BA1 is: 'Allele frequency is too high for the disorder (Stand-alone)'. The allele frequency is 0%, not above threshold. Therefore, this criterion is not applied.
BS1 (Not Applied)
According to standard ACMG guidelines, the rule for BS1 is: 'Allele frequency is greater than expected for the disorder (Strong)'. The allele frequency is 0%, below any threshold. Therefore, this criterion is not applied.
BS2 (Not Applied)
According to standard ACMG guidelines, the rule for BS2 is: 'Observed in healthy individuals with full penetrance expected at an early age (Strong)'. There is no evidence this variant is observed in healthy individuals. Therefore, this criterion is not applied.
BS3 (Not Applied)
According to standard ACMG guidelines, the rule for BS3 is: 'Well-established functional studies show no damaging effect on protein function or splicing (Strong)'. Functional studies demonstrate damaging (gain-of-function) effects. Therefore, this criterion is not applied.
BS4 (Not Applied)
According to standard ACMG guidelines, the rule for BS4 is: 'Lack of segregation in affected family members (Strong)'. No segregation data exist. Therefore, this criterion is not applied.
BP1 (Not Applied)
According to standard ACMG guidelines, the rule for BP1 is: 'Missense variant in a gene where only loss of function causes disease (Supporting)'. This variant is truncating. Therefore, this criterion is not applied.
BP2 (Not Applied)
According to standard ACMG guidelines, the rule for BP2 is: 'Observed in trans with a pathogenic variant for a dominant disorder or in cis with a pathogenic variant (Supporting)'. No such observations are reported. Therefore, this criterion is not applied.
BP3 (Not Applied)
According to standard ACMG guidelines, the rule for BP3 is: 'In-frame deletions/insertions in a repetitive region without known function (Supporting)'. This variant is a frameshift deletion. Therefore, this criterion is not applied.
BP4 (Not Applied)
According to standard ACMG guidelines, the rule for BP4 is: 'Multiple lines of computational evidence suggest no impact on gene or gene product (Supporting)'. Only splicing algorithms were run and predicted no effect; overall computational evidence is insufficient. Therefore, this criterion is not applied.
BP5 (Not Applied)
According to standard ACMG guidelines, the rule for BP5 is: 'Variant found in a case with an alternate molecular basis for disease (Supporting)'. No alternate molecular explanation is reported. Therefore, this criterion is not applied.
BP6 (Not Applied)
According to standard ACMG guidelines, the rule for BP6 is: 'Reputable source reports variant as benign, but without accessible evidence (Supporting)'. No reputable source classifies this variant as benign. Therefore, this criterion is not applied.
BP7 (Not Applied)
According to standard ACMG guidelines, the rule for BP7 is: 'Synonymous variant with no predicted impact on splicing (Supporting)'. This variant is not synonymous. Therefore, this criterion is not applied.